
Peripheral arterial disease, or PAD, is a relatively common occurrence as we age. In fact, by the age of 80, about a quarter of men and 20% of women have it, and it is estimated that over 6 million people in the United States suffer from PAD. PAD involves the narrowing or blockage of the arteries that carry blood to the extremities, especially the legs. This is due to atherosclerosis, the buildup of plaque within the blood vessel. While the peripheral arteries exist in the arms as well, PAD is far more common in the legs.
The risk of PAD begins at about age 40, during which time women have a greater risk than men. By the age of 60, the risk of PAD in men is higher versus that of women. PAD is a progressive disease, meaning that it does not get any better without intervention. As such, an early diagnosis and treatment plan will allow for the best outcomes.
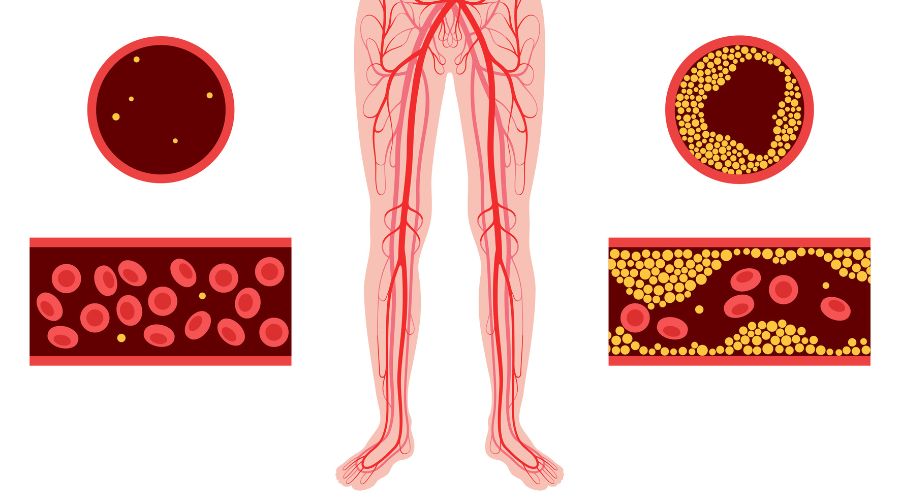
The Causes of PAD
There are several modifiable and non-modifiable factors that can cause PAD. Modifiable factors include leading a sedentary lifestyle, using tobacco, being overweight or obese, having high blood pressure or high blood cholesterol, or suffering from type two diabetes. Some patients may have family histories that increase the risk of PAD. African Americans have a higher risk of PAD as do those of Hispanic descent.
The Signs and Symptoms of PAD
The most common symptom of PAD is pain when walking or performing other physical activities using the legs. Often, the pain improves significantly with just a bit of rest. Interestingly, upwards of half of PAD patients have no leg symptoms at all. There are also outward physical signs of PAD, including muscle weakness, numbness in the feet or toes, ulcers that do not heal easily, decreased pulse in the lower extremities, hair loss, shiny skin, and skin that is cool or cold to the touch.
How We Diagnose PAD
Based on a complete medical history and a physical examination, we can often make a preliminary diagnosis of PAD. However, it is important to have an objective test-based understanding of the disease. We may perform a series of tests including an Ankle Brachial Index, which compares the blood pressure of the ankles to that of the arms when at rest and after exercise. We may also collect data via Magnetic Resonance Angiography, or CT angiography.
Treating PAD
Depending on the severity of PAD, we may pursue several conservative options to improve the patient’s lifestyle and reduce symptoms. This will include improving diet and exercise habits, reducing cholesterol and blood pressure levels, and increasing blood flow to the extremities. We may also prescribe blood thinning medication to help blood pass through the narrowed artery more easily. Patients may require cholesterol and blood pressure lowering medication. If lifestyle change and medication do not show an appreciable improvement in symptoms, surgery to bypass the affected artery may be necessary.